Unlocking the Gut-Brain Connection: A Pathway to Wellness
Your Health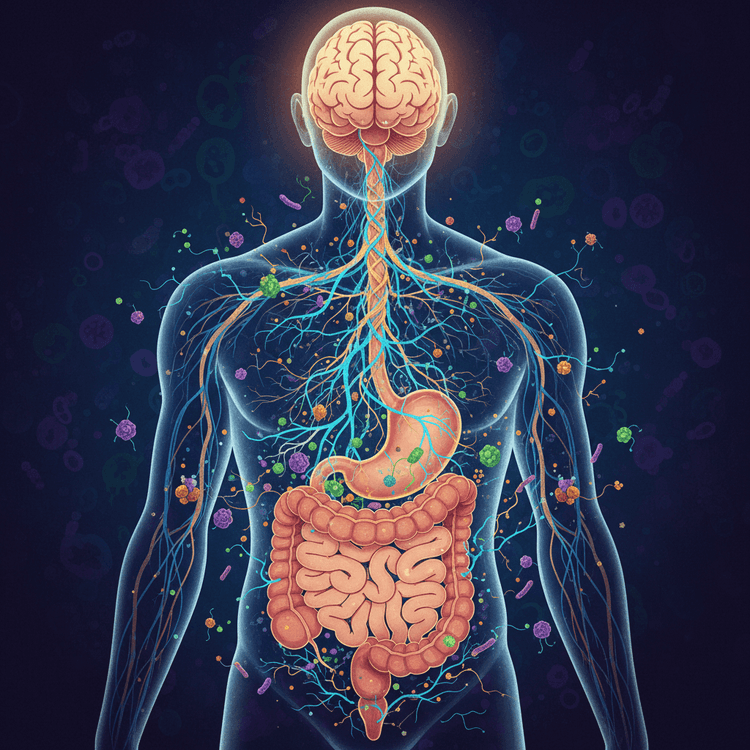
Explore the intricate gut-brain connection and understand how your digestive health profoundly impacts mental well-being. Discover the science behind this vital axis. The profound and often underestimated relationship between our gut and brain, famously known as the gut-brain axis, is a fascinating frontier in health science. This complex bidirectional communication system constantly exchanges information, influencing everything from our mood and cognitive function to our stress response and overall mental health. Far from being isolated entities, our digestive system, often dubbed our "second brain" due to its extensive enteric nervous system (ENS), is intimately linked to the central nervous system (CNS). This connection is mediated by a sophisticated network involving neural pathways, hormones, and the immense population of microorganisms residing in our gut, collectively known as the gut microbiome. Understanding this intricate interplay is crucial for anyone seeking to optimize their well-being, as emerging research consistently highlights how disturbances in one can manifest as issues in the other. From anxiety to depression, and even neurodegenerative conditions, the health of your microbiome and the integrity of the gut lining play pivotal roles, making the gut-brain connection a cornerstone of holistic health.
The Bidirectional Highway: How the Gut-Brain Axis Communicates
The communication between the gut and the brain is not a one-way street but rather a bustling, bidirectional highway, predominantly facilitated by the vagus nerve. This cranial nerve acts as a superhighway, transmitting signals from the brain to the gut and, critically, from the gut back to the brain. Beyond neural pathways, the gut microbiome plays a central role in synthesizing crucial neurotransmitters, such as serotonin (an impressive 90% of the body's serotonin is produced in the gut) and dopamine, which significantly influence mood, sleep, and appetite. When the gut microbiome is balanced and diverse, it supports healthy neurotransmitter production, contributing to mental resilience. Conversely, an imbalance, known as dysbiosis, can lead to reduced neurotransmitter availability and an increase in inflammatory compounds that can cross the blood-brain barrier, affecting cognitive function and emotional regulation. For example, studies have shown that individuals with certain mood disorders often exhibit distinct microbial profiles compared to healthy individuals. The gut's immune system also interacts closely with the brain, with gut inflammation potentially triggering systemic inflammation that can impact brain health. This intricate network means that what happens in your gut doesn't just stay in your gut; it profoundly influences your brain's structure and function, helping to answer how the gut can influence our thoughts and feelings.

Optimizing Your Gut for Enhanced Mental Well-being
Given the profound influence of the gut-brain connection, optimizing your gut health is a powerful strategy for enhancing overall mental well-being. A foundational step is adopting a diet rich in fiber, prebiotics, and probiotics. Foods like fermented vegetables, yogurt, kefir, and kombucha are excellent sources of beneficial bacteria, which can enrich your gut microbiome and support the production of feel-good neurotransmitters. Integrating prebiotic-rich foods such as garlic, onions, bananas, and oats provides essential fuel for these beneficial microbes. Beyond diet, managing stress effectively is paramount, as chronic stress can negatively impact gut barrier integrity and alter microbial composition. Techniques like mindfulness, meditation, regular exercise, and adequate sleep all contribute to a healthier gut environment. For example, a Mediterranean-style diet, abundant in fruits, vegetables, whole grains, and healthy fats, has been consistently linked to better mental health outcomes, likely due to its positive impact on the gut microbiome. Consider incorporating diverse plant-based foods to promote a wider array of beneficial bacteria. These lifestyle changes not only alleviate digestive issues but also foster a more resilient brain, demonstrating how simple dietary and lifestyle shifts can profoundly improve your mood and cognitive function by nurturing your internal ecosystem.

Discussion
No comments yet
Be the first to share your opinion!
Jennifer Trimbee
Aug 19, 2025

0 reading now
What Causes Cysts and When to Worry
Cysts are fluid-filled sacs that can develop in various parts of the body, including the skin, ovaries, and internal organs. They are usually benign, meaning they are not cancerous, and are often caused by blockages in ducts, cell proliferation, or infections. Hormonal changes, genetic factors, and chronic inflammatory conditions can also contribute to cyst formation. While most cysts are harmless and may resolve on their own, some can become problematic if they grow large, cause pain, or become infected. It's important to monitor cysts and seek medical advice if they change in size, color, or sensation, or if they occur in conjunction with other symptoms.
Read more
Jennifer Trimbee
Aug 19, 2025

Disclaimer
This site offers information designed for educational purposes only. You should not rely on any information on this site as a substitute for professional medical advice, diagnosis, treatment, or as a substitute for, professional counseling care, advice, diagnosis, or treatment. If you have any concerns or questions about your health, you should always consult with a physician or other healthcare professional.

